Parshat Ki Tisa – Washing well
There were two maternity hospitals in Vienna on July 1, 1846, when Ignaz Semmelweis was hired to work in the First Obstetrical Clinic. He was a Hungarian – an outsider to Austrian society — and his position was equivalent to a modern chief resident.
Both the First and the Second Obstetrical Clinics had been created as part of a Europe-wide attempt to minimize infanticide. By encouraging women to give birth in hospitals, the government could better monitor the number of children, and it was easier for women to give up unwanted children to orphanages for adoption.
Due to the hospital system, slightly fewer babies died – from an average of over 30 percent in 1834, to under 26% by 1876. And it seems that infanticide also decreased, though there are no clear measures for that.
But the cost was huge – in these maternity hospitals the number of women who died due to complications from childbirth skyrocketed.
About five out of 1,000 women who gave birth at home died in childbirth. But the Second Clinic had an average mortality rate of seven percent, or 70 out of every 1,000. However, the First Clinic was far worse – 16% of women who went there never came out alive. (These are an average of Semmelweis’s own numbers. The actual mortality rates varied from month to month. What is certain is that the First Clinic had a significantly higher death rate than the Second clinic).
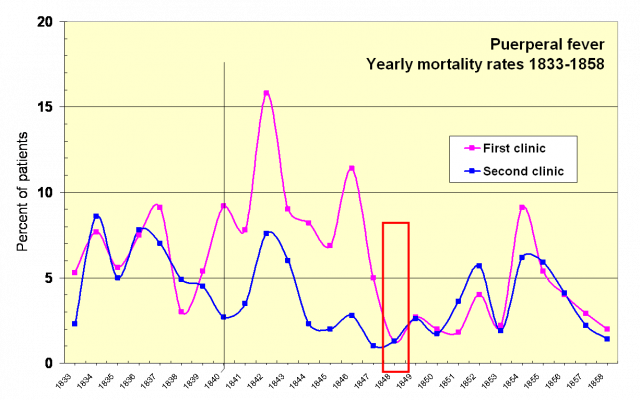
The expectant mothers themselves knew how dangerous the First Clinic was. Semmelweis wrote (in The Etiology, Concept, and Prophylaxis of Childbed Fever p. 69):
Because of the bad reputation of the first clinic, everyone sought admission to the second clinic. For this reason,… if the second clinic began to admit, within a few hours it was necessary to resume admitting patients to the first clinic because the passageway was crowded with such a great number of persons awaiting admission to the second clinic. In a short time, all the free places were taken. In the five years I was associated with the first clinic, not once did overcrowding make it necessary to reopen admission to the second clinic.
And on p. 70 Semmelweis wrote:
Frequently one must witness moving scenes in which patients, kneeling and wringing their hands, beg to be released in order to seek admission to the second clinic.
The cause of death was almost always from what was referred to as childbirth fever, or puerperal fever. This horrific, painful and speedy illness was described by Dr John Leake in his 1775 book, Practical Observations on the Child-bed Fever: and also on the Nature and Treatment of Uterine Hemorrhages, Convulsion, and such other Acute Diseases (pp. 45-46)
The Childbed Fever generally commenced about the evening of the second or beginning of the third day after delivery, with a rigor or shivering fit. Sometimes it came on sooner, and at other times, though rarely, it has been known to appear as late as the fifth or sixth day. In many women, the attack was sudden, without any apparent cause or preceding indisposition; and soon followed by headache, restlessness, great sickness at the stomach and bilious vomitings.
What caused such a horrible illness? Semmelsweis (on p. 112) summarized the prevailing wisdom at the time:
From the first medical writers on, from Hippocrates until the most recent times, it was the unchallenged conviction of all physicians of all times that the horrible ravages of childbed fever among maternity patients were epidemic – that is, they were due to atmospheric influences. Influences that, notwithstanding every possible precaution of the physician, ravaged unabated and without remission.
Leake explained, (p. 27):
That women, after delivery, are more disposed to fever at one time than another, according to the constitution of the air, cannot be doubted.
A few years later, Dr Charles White, in his 1791 book A Treatise on the Management of Pregnant and Lying-In Women wrote (pp. 286-287):
A true puerperal fever is originally caused by a putrid atmosphere or too long confinement of the patient in a horizontal position.
The Scottish physician William Cullen, author of many medical textbooks, wrote that it was due to the effects of certain “noxious powers.”
Many also thought the disease was brought about due to the mothers’ emotional state. Leake wrote:
Now and then, this fever seemed to be brought on by catching cold, or errors in diet, but much oftener by anxiety of mind; and therefore, women of delicate constitutions, who are very susceptible and continually agitated by hopes and fears, are, of all others, the most subject to it, and recover with the greatest difficulty; consequently, unmarried women, for obvious reasons, were very apt to be seized with it.
Semmelweis had learned all these theories in medical school. But after he saw the huge discrepancy in mortality numbers between the two almost identical clinics, he rejected them. He reasoned that the atmosphere must have been equally “putrid” in both clinics, and the mothers had equally long horizontal confinements.
He accepted that the women in the First Clinic were much more agitated and anxious – mainly because they knew they had a greater chance of dying there than in the Second Clinic. But this could not explain the differences.

He spent months carefully examining all the other the seemingly trivial differences between the two maternity hospitals to try and identify the cause of the deaths.
The First Clinic was staffed by doctors and medical students (all male). The Second Clinic was staffed by midwives and nurses (all female). But surely, he reasoned, having expert male doctors was to the benefit of the mothers in the First Clinic.
Perhaps the fever was caused by overcrowding. Except that the Second Clinic was far more overcrowded than the First. It could not be due to epidemics raging outside the hospital walls, because he noted that many women didn’t make it to the clinics in time and gave birth in the street. They too, had a higher survival rate than women who gave birth in the First Clinic (the truth is that many of them intentionally delivered their baby on the grubby sidewalks of Vienna, rather than risk death at the First Clinic).
Semmelweis looked at the diets of the women in the two clinics, and their general treatment, but could find no significant difference. Perhaps, he reasoned, the male doctors were more forceful when they examined the women than the midwives in the Second Clinic, but he also discounted that.
He noted that in the First Clinic, the priest administering the last rites to dying mothers would walk ringing a bell through five wards before reaching the patients, whereas in the Second Clinic the priest had direct access to the maternity ward. Perhaps this had a psychological affect on the women, causing them to die. So he had the priest change his route, and enter without ringing the bell, but that made no difference.
He described himself “like a drowning man clutching at straw” when he noted that in the First Clinic women gave birth lying on their backs, whereas in the Second Clinic they were on their sides. He persuaded the doctors in the First Clinic to also deliver women laterally, but again, this made no difference.
After almost a year, a tragic accident gave him a clue. The morgue was in the same building as the First Clinic, and medical students would begin their days by conducting autopsies of recently deceased patients, before doing their rounds and delivering babies.

Semmelweis’s colleague and professor, Jacob Kolletschka, was accidentally stabbed in the finger by a student with a scalpel during an autopsy he was conducting. Within a few days, Kolletscka was dead, and Semmelweis was ordered to do conduct a postmortem examination.
Semmelweis realized that Kolletscka had exhibited almost identical symptoms to the women who died of childbirth fever.
He theorized that there must be some “cadaverous particles” or “morbid poison” that doctors were getting on their hands during autopsies. And that they were transferring this poison to the women they were treating.
Nowadays, we know that puerperal fever is caused by bacterial infection. But germ theory was not yet known and Semmelweis had no explanation for the mechanism by which the disease was being transferred, Semmelweis concluded that the women were dying from some type of “putrid organic matter” that was being spread from the diseased bodies of the dead to living healthy women.
He instructed the doctors and students to start washing their hands between leaving the morgue and treating the patients. Unfortunately, no soap was available, but Semmelweis found chlorinated lime – a bleaching agent – and had them wash with that.
The results were immediate and spectacular. Within weeks, the mortality rate in the First Clinic was down to less than that of the Second Clinic.
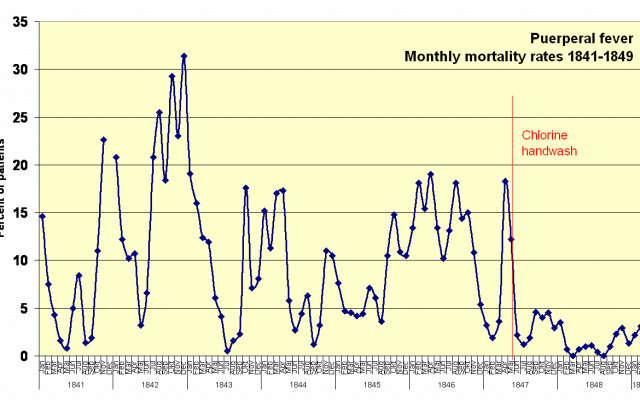
And the number of deaths continued to fall. In June only 2.2% of women died, in July only 1.2%, and in two months in the year following his discovery, the death rate was zero.
Semmelweis was convinced. He started lecturing on the benefits of hand washing and trying to spread the word.
But, despite his empirical proof that washing hands saved lives, the other doctors and hospitals refused to listen to him. Why should they listen to this Hungarian, when Vienna had the best doctors? Why should they wash with bleach, which stung and chafed their hands? And how dare this impudent foreigner imply that they were dirty?
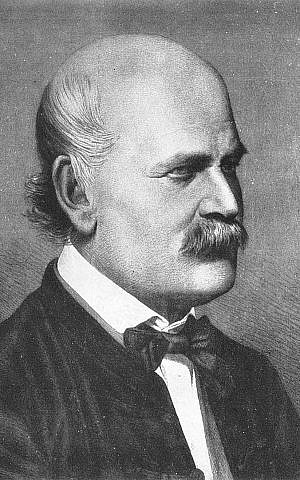
Semmelweis was ridiculed and rejected. He lost his position at the First Clinic and was forced to return to Budapest. There he wrote a book on the importance of hand washing, but it was so badly written (and not edited) that it was almost unintelligible.
The doctor became more and more passionate about his cause. Because nobody would listen to him, he began writing angry letters to prominent obstetricians across Europe, calling them irresponsible murderers.
His family feared he was losing his sanity. In 1865 they tricked him into entering an insane asylum. When he tried to escape, he was caught and beaten by the guards. His wounds were tended to by a doctor, who almost certainly didn’t wash his hands first, and Semmelweis died two weeks later of sepsis – the very disease he had tried to prevent. He was 47 years old.

This week’s Torah portion, Ki Tisa, stresses the importance of hand washing. It states (Exodus 30:18-21):
You shall make a basin of brass, with a brass bass, for washing; and you shall place it between the Tent of Meeting and the altar, and you shall place water in it. And Aharon and his sons shall wash their hands and their feet with it. When they enter the Tent of Meeting, they shall wash their hands so that they not die… They shall wash their hands and their feet so that they do not die, and it shall be an eternal statute for him and his children for all generations.
This obviously only applied to the priests before they performed the service in the Temple. But washing for purification became part of Jewish life – the priests had to wash their hands before eating the terumah they were given. And later on, all Jews adopted the custom of washing their hands before eating bread as a reminder of the priests and their terumah.
But if we look a little deeper, there is a more profound message in the basin.
The Torah says (Exodus 38:8) that it was made from the mirrors.
He made the brass basin and its base of brass, from the mirrors of the women who had made legions, who gathered at the entrance to the Tent of Meeting.
Rashi on the verse explains (citing a midrash) that Moses initially did not want to accept these mirrors. He felt that mirrors used by the women to beautify themselves and seduce their husbands were inappropriate to have within the holy Tabernacle.

But God said that these mirrors “are more precious to me than anything else.” Because it was with these mirrors that the women built up the Israelite nation despite the hardship of slavery.
The men were exhausted from their forced labor. But the women would come and greet them, bringing them food and drink. Then each wife would take out her mirror, gaze into it, and proclaim that she was more beautiful than her husband. One thing would lead to another, and the women became pregnant.
And, the midrash adds, that because the mirrors were initially used for this purpose, the basin was later used to bring peace between husbands and wives.
Looking into a mirror is a brave thing to do. Usually, when we look at one another, we see the totality of the person. But when we stare into a mirror, we see all our faults and flaws in close detail.
The women in Egypt used the mirrors to reflect not on themselves, but on their relationship with their husbands and with the world. The men felt there was no point in having children, because they were doomed to a life of slavery. The women challenged the assumptions of the men using the mirrors.
But rather than contradicting or arguing with their husbands, they first took a good look at themselves. Were they right in their views? Or were they merely acting without thought based on the certainty of the ignorant?
By examining and challenging themselves first they were then able to convince their husbands that the exile would end, and the slavery was only temporary.
Semmelweis’s contemporaries ignored his evidence because they had foolish conviction that they were right. It made no difference that the evidence, and the death rate, proved them wrong. They were certain that Semmelweis could not be right, for if he was, it would challenge everything they knew about medicine and the world.
This was the symbolism of the basin made of mirrors in the Temple. Challenging everyone to examine what they thought they knew and reflect on whether it was the most beautiful and correct.
While researching Semmelweis, I did find some people who wrote that his ideas were not accepted due to anti-Semitism. However, I did not find any evidence that he was Jewish. This Letter to the Editor makes a strong case that he was born and died a Roman Catholic. And his grave shows no indication that he was Jewish.
There is an excellent podcast on Semmelweis from the amazing The Constant. Check it out.
—
I’ve started sharing more of my Torah thoughts on Facebook. Follow my page, Rabbi Sedley.





