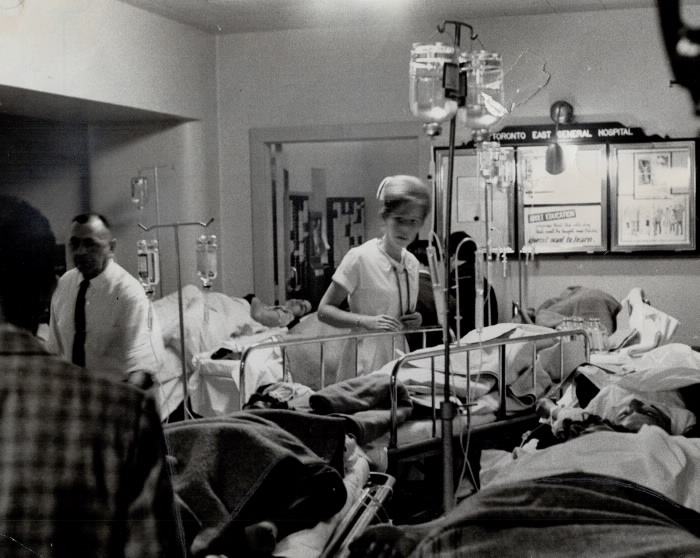
Life and death in the corridors
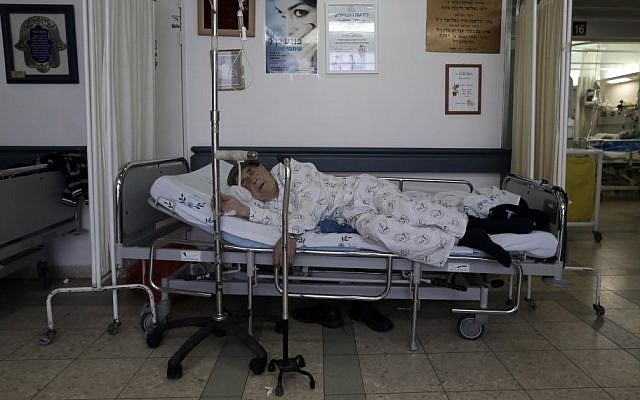
In 1906 Upton Sinclair wrote The Jungle describing the incredulous conditions in the meat factories of Chicago. As a kid, reading this book had a deep impact on me. I was amazed at how one book could illuminate so much that was wrong. Unfortunately, here in Israel, we also have a crisis which has been brewing for many years. Though many articles have been written about it, major changes have not been forthcoming. I am speaking about the state of hospital care in Israel and what many professionals have called a “life-threatening emergency”. Unfortunately most of the candidates in our upcoming election have not addressed this crisis.
For the last year I had a few hospital experiences that opened my eyes. I witnessed overworked nurses doing their best in near-impossible conditions. I was often under stress with no one to call or consult. I was lucky if a doctor visited me. I witnessed the dedication of the hospital’s “unsung heroes”: the nurses. Sometimes they smiled, sometimes they didn’t. But one thing was clear, the nurses were clearly under extreme stress, sometimes at the breaking point.
Between 2013 and 2019 a number of articles were written on this subject. On January 13, 2013 the HaAretz headlines read: “Israel’s Hospitals Are Overcrowded Year Round, Not Just in Winter. Although the population is both aging and growing, the Health Ministry has added few beds, leaving more patients in hospital hallways.”
In Times of Israel, May 5, 2015 the headlines read: Comptroller slams hospitals for bed shortages, poor conditions; Lack of emergency doctors heightens risk of misdiagnosis while medical tourism takes resources from Israeli patients – report.
In the Jerusalem Post on January 19, 2019 the headlines read: “Conceptual revolution’ required to end hospital ward overcrowding; According to data provided by the Health Ministry the nationwide average occupancy of internal medicine wards stands at approximately 114% of their capacity.”
Over the last six years, essentially nothing has changed. It has gone from bad to worse!
And in Great Britain, for instance? In the BBC News on January 8, 2018, Patients Dying in Corridors the headlines read: “Patients are dying in hospital corridors as safety is compromised by “intolerable” conditions, doctors say.”
My personal interest in the subject was recently renewed by several encounters with health professionals, primarily nurses, and chronically-ill patients who went through horrifying experiences. What I heard from them was beyond belief. If we were living in third-world country it might be understandable, but as our leaders tell us, we are one of the most technologically-advanced countries in the world and the eighth “most powerful”.
My recent meeting with a veteran nurse working at one of Jerusalem’s major hospitals was my most powerful eye-opener. For her protection, her name will remain anonymous, but for ease of reading I will refer to her as “Sue”. I must also preface that whatever I quote from Sue has been corroborated from my own experiences as a hospital patient, experiences which I had forgotten (apparently through their traumatic nature). They have now risen to the surface.
Sue is one of the dedicated nurses we are privileged to have in the hospital system; such nurses work long hours, sometimes under unbearable conditions. The current picture is one of overcrowding, life-threatening mistakes, supervisory negligence, lack of proper equipment, lack of time for carrying out necessary tasks, including basic human contact ( i.e. “bedside manner”) something proven to be as healing as a “thousand clowns” and even medications.
The most shocking of Sue’s revelations was her description of the ill-equipped hospital corridors which have, in effect, become hospital “rooms”. Sue provided the following “picture”:
“The morning shift is when it all happens; it is also the busiest shift. In the morning I’ll usually come in and there already will be several people in the corridor; this is not good because you know that you’ll be receiving more like that. This is because the ER (emergency room) will be receiving people throughout the day. You may be seeing some of these patients in the corridor for the first time, where they may have already spent 2-3 days there; they want to know what’s going on. If they arrived on a Thursday night and there were no discharges on Sunday morning they would just stay in the aisles. The ER simply can’t keep them.”
“If a person in the corridor needs urgent help, like needing to be resuscitated, someone will need to be kicked out of a room to accommodate the emergency. Often the ER will ship us patients that they call stable and that is nothing short of a lie. That’s a common phenomenon all over Israel. If a person is on a oxygen balloon and runs out, sometimes a nurse will not know that; because the corridor is not a room, nothing will buzz.”
“So the corridor is a sort of no-man’s land?” I ask.
Sue responds: ” Yes, absolutely. The nurse will usually get to those patients last. As a patient, unless you know the right people, you are in trouble. For instance I had a patient in the corridor who had been there over the weekend and he was OK, but I guess something happened over the night because the next morning he had deteriorated rapidly; his family brought in a famous cabinet minister and within two hours he was moved to ICU (Intensive Care Unit). I am happy for that person. But if that hadn’t happened, he would have deteriorated . Because of the crowded conditions, I physically couldn’t get through to him with my cart to give him his meds; my cart was too wide for the remaining corridor space. I would carry my meds by hand, which is grounds for making mistakes. He had to have a blood transfusion. Patients who receive a transfusion need to be monitored much more carefully because of possible life threatening side effects; of course that can’t happen at the end of the corridor!… In the end, it was only because of who the patient’s family knew, that he was whisked away. That family was lucky because they pulled the right strings at the right time.”
She continues: “I usually come into to a bunch of tired, angry patients and family members who are in the corridor. The night nurse on the shift briefs me about all the patients. Soon I get more ‘kabbalot’, and then the horror stories happen throughout the morning.” Sue later explains that people who yell and scream eventually get the attention, while the more polite ones are easily overlooked. The nurses and doctors are simply afraid to speak out in public. They are afraid of their jobs and professional status. What they see is a lopsided system which patients and their families can only “beat” by screaming and yelling until they get what they need. People who are polite most often are at the end of the “care chain”.
And what of burn out? There are real reasons. She explains: “I have heard from another nurse that in the USA the average patient-nurse ratio is maximum 8 to 1, where here it is at least 12 to 1, but can easily go up to 17 to 1.” Actually according to research, even the 8:1 ratio is considered dangerous! The NY state nurses association provides the following information:
Safe Staffing saves lives
- Hospitals that staff 1:8 nurse-to-patient ratios experience five additional deaths per 1,000 patients than a 1:4 nurse-to-patient ratio (Journal of the American Medical Association, 2002).
- The odds of patient death increases by 7% for each additional patient the nurse must take on at one time (Journal of the American Medical Association, 2002).
- Outcomes are better for patients when staffing levels meet those established in California, including an increase in lives saved, shorter hospital stays, and general improvement in quality care (Health Services Research, 2010).
I then ask Sue the obvious: “People in the corridors, how is their care endangering them?” Sue responds: “It may not endanger them but it certainly compromises their level of care. On a good day I’ll see them twice during an entire shift. And I will get to them much, much later, so their meds will given to them LAST. Instead of receiving their morning meds at 7:30 AM, I will get to them at 9:30-10. For their meds of 12 noon, I will get to them last. It’s more complicated if they are diabetic. I have to check their blood sugar but I won’t get to them until way after their lunch, when their sugar level will be higher. They will receive a high level of insulin, setting them off track.”
She continues: “And if what if a patient HAS no one (i.e. family or loved ones)? Recently there was one patient lying in the corridor and she stopped breathing; no one noticed her. The cleaning woman came and happened to take a look at the patient; of course it’s not her responsibility. They eventually resuscitated he in the corridor, which is unthinkable situation; that’s not supposed to happen! We try to take privacy seriously. Sometimes we have to insert a catheter or perhaps change someone’s diaper. With people whizzing by, how can we maintain a minimal standard of privacy?”
I ask: Where’s the breaking point?” She answers. “When a nurse makes a mistake that puts a patient’s life in danger. And that actually has happened recently.” She chooses not to elaborate.
“But I’ll tell you something else that happened. The rooms were originally designed for two beds with two oxygen outlets per room, but now there are three beds. Often there three people who need oxygen, with only two oxygen outlets! But one night we were only three nurses and there was someone with a ventilator in the middle of the room; someone had removed the tube. The following morning one of the staff found the oxygen tube on the floor!
“What had actually happened?: In the middle of the night a patient needed CPR (Cardiopulmonary resuscitation) while the patient next to him was also connected to an oxygen device of sorts. Amid the attempts to save the guy in the middle of the room (with very little space to squeeze by to perform the CPR) the oxygen tube belonging to the other patient was accidentally yanked from the oxygen source in order to accommodate the critical CPR patient. This happened because both of the patients who were completely dependent on oxygen, were sharing ONE oxygen unit.” Sue adds that recently all the rooms were finally equipped with three oxygen outlets.
I finally ask, “Sue, aren’t there standards?” She begins to describe the hospital accreditation procedure.
“It’s somewhat of a bluff and everyone knows it, from all the doctors to the maintenance staff. JCI (Joint Commission International) oversees the Accreditation process; an international group of representatives go around for a week interviewing, checking and looking around to make sure that everything is up to international standards. Leading up to that visit, the hospital sort of turns itself over and all of a sudden everything works like clockwork. No one lays in the corridor because MADA (Magen David Adom emergency services) is instructed not to bring people to the hospital. It’s not real. After the commission leaves some of the improvements “hold up” for a while, because people basically want to maintain a certain standard of care, but of course eventually things slowly return to their “natural” lacking state.”
According to Sue, after accreditation visit the empty corridors eventually become fill up. The generously-supplied medication cabinets again become lacking, and once again nurses found themselves frantically searching other wards for the much-needed meds. Ample supply of nurses on every shift finally diminishes. The cleaning staff of the hospital, having been expanded, returns to bare minimum. The sparkling clean hospital returns to its “normal” state. Though the hospital passed with flying colors, eventually things returned to how they were before the accreditation visit.
Jokingly I say to her “Your work is like the man in the circus spinning saucers on a series of poles; your energy is spent moving from one patient to another, with no time to stop, to breath, to engage in polite and healing conversation with the patient.” She smiles. But this is a serious matter. Sub-standard conditions have brought about a state of chronic nurse fatigue and burn out, certainly something that should trigger “red lights”. Many nurses simply cannot function at this inhuman pace and intensity, and if they DO, at some point they find themselves making mistakes, sometimes life threatening.
None of us will be spared. I can hear the voices out there saying, “Well, I pay extra to my health fund, so this will not effect ME”. Wrong. What we are looking at is a crisis which will effect us all, rich or poor; we expect to get older and have top quality hospital care, but what is now accumulating is a universal acceptance for sub-standard care which, as time moves on, will become more and more prevalent.
Where are the politicians when we need them? Who is addressing this issue? Who can we elect that will promise to alleviate this now life-threatening, inhumane travesty? Time (and our elections) will only tell!
Life and death in the corridors: also an international problem!….
Embed from Getty Images